|
STATISTICAL BRIEF #302
December 2022
Audrey J. Weiss, Ph.D., Michael A. Head, M.S., and Lawrence D. Reid, Ph.D., M.P.H. Introduction Mental health disorders are common during and following pregnancy and may contribute to poorer maternal and neonatal outcomes.1 For example, maternal depression is associated with a higher rate of premature delivery and low birth weight infants.2 The proportion of delivery hospital stays involving a mental health disorder diagnosis has increased from 0.6 percent of delivery stays in 2000 to 7.3 percent of delivery stays in 2018.3 Moreover, this increasing trend was exacerbated in 2020 when pregnant women experienced COVID-19 pandemic-related stress associated with factors such as job loss, feeling unprepared for birth, and fear of COVID-19 infection.4–6 The prevalence of mental health disorders is generally similar across racial and ethnic groups in the United States.7 However, little is known about racial and ethnic differences in the rates of mental health disorders among women during pregnancy and delivery. Given the high prevalence of mental health disorders among delivery stays, especially during the COVID-19 pandemic, it is important to understand how mental health disorder diagnoses differ by patient race and ethnicity in order to address existing disparities and prevent widening disparities among maternal and neonatal outcomes. This Healthcare Cost and Utilization Project (HCUP) Statistical Brief presents statistics on mental health disorders during delivery inpatient stays by patient race and ethnicity using weighted estimates from the 2020 National Inpatient Sample (NIS). First, changes in the rate of delivery stays with any mental health disorder diagnosis are presented by patient race and ethnicity from 2017 to 2020. Second, the distribution of delivery stays with and without a mental health disorder diagnosis is presented by patient race and ethnicity. Third, the rate of delivery stays with any mental health disorder diagnosis is presented by patient race and ethnicity for select patient and hospital characteristics and for specific and prevalent mental health disorders. Finally, the rate is provided by patient race and ethnicity for delivery stays involving common obstetric risk factors and either a concurrent mental health disorder diagnosis or no concurrent mental health disorder diagnosis. Because of the large sample size of the NIS data, small differences can be statistically significant but not clinically important. Thus, only differences greater than or equal to 10 percent are discussed in the text. Findings Prevalence of mental health disorder diagnoses among delivery stays, by patient race and ethnicity, 2020 Figure 1 displays the rate of delivery stays involving at least one mental health disorder diagnosis per 100 delivery stays from 2017 to 2020. |
|
Figure 1. Rate of delivery stays involving a mental health disorder diagnosis, by patient race and ethnicity, 2017–2020
Abbreviations: API, Asian/Pacific Islander; NH, non-Hispanic Line graph showing the rate of delivery stays involving at least one mental health disorder diagnosis per 100 delivery stays by patient race and ethnicity from 2017 to 2020. Overall: 2017, 6.9 per 100 delivery stays; 2018, 7.9; 2019, 9.1; 2020, 10.5. Asian/Pacific Islander non-Hispanic (NH): 2017, 2.2 per 100 delivery stays; 2018, 2.6; 2019, 2.9; 2020, 3.6. Black NH: 2017, 5.8 per 100 delivery stays; 2018, 6.6; 2019, 7.5; 2020, 8.5. Hispanic: 2017, 3.8 per 100 delivery stays; 2018, 4.6; 2019, 4.9; 2020, 5.9. White NH: 2017, 9.1 per 100 delivery stays; 2018, 10.6; 2019, 12.2; 2020, 14.0. Other NH: 2017, 4.5 per 100 delivery stays; 2018, 5.1; 2019, 6.4; 2020, 7.7.
|
|
|
Figure 2 presents the distribution of delivery stays with and without a mental health disorder diagnosis in 2020 by patient race and ethnicity. Figure 2. Distribution of delivery stays with and without a mental health disorder diagnosis, by patient race and ethnicity, 2020
Abbreviations: API, Asian/Pacific Islander; MHD, mental health disorder; NH, non-Hispanic Bar chart showing the distribution of delivery stays with and without a mental health disorder diagnosis by patient race and ethnicity in 2020. Delivery stays with a mental health disorder (N=361,700): Asian/Pacific Islander non-Hispanic (NH), 2.0%; Black NH, 11.9%; Hispanic, 11.6%; White NH, 67.8%; other NH, 3.7%; missing, 3.0%. Delivery stays without a mental health disorder (N=3,092,200): Asian/Pacific Islander NH, 6.2%; Black NH, 15.0%; Hispanic, 21.7%; White NH, 48.6%; other NH, 5.1%; missing, 3.3%.
|
|
|
Table 1 presents the rate of delivery stays with a mental health disorder diagnosis per 100 delivery stays by patient race and ethnicity across select patient and hospital characteristics in 2020.
Table 1. Number and rate of delivery stays with a mental health disorder diagnosis per 100 delivery stays, by patient and hospital characteristics and patient race and ethnicity, 2020 |
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
|
Figure 3 displays the rate of delivery stays involving the two most common mental health disorders of the 13 examined in 2020. Figure 3. Rate of delivery stays involving a mental health disorder diagnosis, by type of mental health disorder and patient race and ethnicity, 2020
Abbreviations: API, Asian/Pacific Islander; NH, non-Hispanic Bar chart showing the rate of delivery stays involving the two most common mental health disorders of the 13 examined by patient race and ethnicity in 2020. Data are provided in Supplemental Table 1.
|
|
|
Maternal risk factors among delivery stays involving a mental health disorder diagnosis, by patient race and ethnicity, 2020
Table 2 presents the rate of delivery stays involving 12 common obstetric risk factors among delivery stays with and without a co-occurring mental health disorder diagnosis by patient race and ethnicity in 2020.8 Risk factors are listed from highest to lowest rate of delivery stays with a co-occurring mental health disorder for all races and ethnicities in 2020. Only risk factors with at least 5 percent prevalence across all racial and ethnic groups are included. Table 2. Rate of delivery stays with obstetric risk factors per 100 delivery stays, by presence of a co-occurring mental health disorder diagnosis and patient race and ethnicity, 2020 |
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
References About Statistical Briefs Healthcare Cost and Utilization Project (HCUP) Statistical Briefs provide basic descriptive statistics on a variety of topics using HCUP administrative healthcare data. Topics include hospital inpatient, ambulatory surgery, and emergency department use and costs, quality of care, access to care, medical conditions, procedures, and patient populations, among other topics. The reports are intended to generate hypotheses that can be further explored in other research; the reports are not designed to answer in-depth research questions using multivariate methods. Data Source The estimates in this Statistical Brief are based upon data from the HCUP 2020 National Inpatient Sample (NIS). Historical data were drawn from the 2017–2019 NIS. Definitions Diagnoses, ICD-10-CM, Clinical Classifications Software Refined (CCSR) for ICD-10-CM/PCS, and diagnosis-related groups (DRGs) The principal diagnosis is that condition established after study to be chiefly responsible for the patient's admission to the hospital. Secondary diagnoses are conditions that coexist at the time of admission that require or affect patient care treatment received or management, or that develop during the inpatient stay. All-listed diagnoses include the principal diagnosis plus the secondary conditions. ICD-10-CM/PCS is the International Classification of Diseases, Tenth Revision, Clinical Modification/Procedure Coding System. There are over 70,000 ICD-10-CM diagnosis codes and 75,000 ICD-10-PCS procedure codes. The CCSR aggregates ICD-10-CM diagnosis codes into a manageable number of clinically meaningful categories.a The CCSR is intended to be used analytically to examine patterns of healthcare in terms of cost, utilization, and outcomes; rank utilization by diagnoses; and risk-adjust by clinical condition. The CCSR capitalizes on the specificity of the ICD-10-CM coding scheme and allows ICD-10-CM codes to be classified in more than one category. Approximately 10 percent of diagnosis codes are associated with more than one CCSR category because the diagnosis code documents either multiple conditions or a condition along with a common symptom or manifestation. All CCSR categories were considered in identifying mental health disorder diagnoses for this Statistical Brief. ICD-10-CM coding definitions for each CCSR category presented in this Statistical Brief can be found in the CCSR reference file, available at www.hcup-us.ahrq.gov/toolssoftware/ccsr/ccs_refined.jsp#download. For this Statistical Brief, a custom version of v2022.1 of the CCSR was used; see below for further details on the differences. DRGs comprise a patient classification system that categorizes patients into groups that are clinically coherent and homogeneous with respect to resource use. DRGs group patients according to diagnosis, type of treatment (procedure), age, and other relevant criteria. Each hospital stay has one assigned DRG. Case definition Inpatient delivery stays were identified using the ICD-10-CM/PCS and DRG codes in Table 3. Delivery stays were defined as records that included a delivery code and did not include an abortion code.
Delivery stays involving a mental health disorder diagnosis were identified based on the presence of any CCSR category listed in Table 4 for any-listed diagnosis on the hospital discharge record. The two specific mental health disorder categories presented in Figure 3 were defined by the following CCSR categories: anxiety and obsessive-compulsive disorders (MBD005 and MBD006) and depressive disorders (MBD002). Among the other CCSR categories involving less common mental health disorders that were not presented in Figure 3, all showed an increase in the rate per 100 deliveries between 2017 and 2020 except for schizophrenia spectrum and other psychotic disorders (MBD001) and somatic disorders (MBD011); however, these two CCSR categories involved very small sample sizes.
Obstetric risk factors were defined with ICD-10-CM codes based on a validated obstetrics comorbidity scoring system developed by Leonard et al.b that used birth data from California during 2016 and 2017 to select 27 patient-level risk factors associated with severe maternal morbidity. Percentage change Percentage change between years was calculated using the following formula: Percentage change = 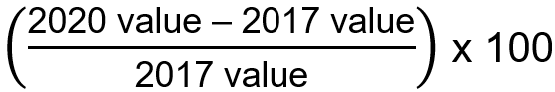
Percentage change between years equals the 2020 value minus the 2017 value divided by the 2017 value multiplied by 100.
Types of hospitals included in the HCUP National Inpatient Sample The National Inpatient Sample (NIS) is based on data from community hospitals, which are defined as short-term, non-Federal, general, and other hospitals, excluding hospital units of other institutions (e.g., prisons). The NIS includes obstetrics and gynecology, otolaryngology, orthopedic, cancer, pediatric, public, and academic medical center hospitals. Excluded are long-term care facilities such as rehabilitation, psychiatric, and alcoholism and chemical dependency hospitals. Beginning in 2012, long-term acute care hospitals are also excluded. However, if a patient received long-term care, rehabilitation, or treatment for a psychiatric or chemical dependency condition in a community hospital, the discharge record for that stay will be included in the NIS. Unit of analysis The unit of analysis is the hospital discharge (i.e., the hospital stay), not a person or patient. This means that a person who is admitted to the hospital multiple times in 1 year will be counted each time as a separate discharge from the hospital. Expected payer To make coding uniform across all HCUP data sources, the primary expected payer for the hospital stay combines detailed categories into general groups:
For this Statistical Brief, when more than one payer is listed for a hospital discharge, the first-listed payer is used. Community-level income Community-level income is based on the median household income of the patient's ZIP Code of residence. Quartiles are defined so that the total U.S. population is evenly distributed. Location of patients' residence Place of residence is based on a simplified adaptation of the Urban Influence Codes (UIC) developed by the United States Department of Agriculture (USDA) Economic Research Service (ERS). Starting with 2014 data, the county-level designation is based on the 2013 version of the UIC. Prior to 2014, the categorization was based on the 2003 version of the UIC. The 12 categories of the UIC are combined into 3 broader categories that differentiate between large metropolitan counties (include one or more urbanized areas with at least 1 million residents), small metropolitan counties (include one or more urbanized areas with 50,000–999,999 residents), and nonmetropolitan counties (i.e., micropolitan counties (include at least one urbanized area with 10,000–49,999 residents) or nonurban residual counties (rural)). Region Region is one of the four regions defined by the U.S. Census Bureau:
Reporting of race and ethnicity Data on Hispanic ethnicity are collected differently among the States and also can differ from the census methodology of collecting information on race (White, Black, Asian/Pacific Islander, American Indian/Alaska Native, Other [including mixed race]) separately from ethnicity (Hispanic, non-Hispanic). State data organizations often collect Hispanic ethnicity as one of several categories that include race. Therefore, for multistate analyses, HCUP creates the combined categorization of race and ethnicity for data from States that report ethnicity separately. When a State data organization collects Hispanic ethnicity separately from race, HCUP uses Hispanic ethnicity to override any other race category to create a Hispanic category for the uniformly coded race/ethnicity data element, while also retaining the original race and ethnicity data. This Statistical Brief reports race and ethnicity for the following categories: Asian/Pacific Islander non-Hispanic (NH), Black NH, Hispanic, White NH, and other NH race and ethnicity (including American Indian/Alaska Native and Other). About HCUP The Healthcare Cost and Utilization Project (HCUP, pronounced "H-Cup") is a family of healthcare databases and related software tools and products developed through a Federal-State-Industry partnership and sponsored by the Agency for Healthcare Research and Quality (AHRQ). HCUP databases bring together the data collection efforts of State data organizations, hospital associations, and private data organizations (HCUP Partners) and the Federal government to create a national information resource of encounter-level healthcare data. HCUP includes the largest collection of longitudinal hospital care data in the United States, with all-payer, encounter-level information beginning in 1988. These databases enable research on a broad range of health policy issues, including cost and quality of health services, medical practice patterns, access to healthcare programs, and outcomes of treatments at the national, State, and local market levels. HCUP would not be possible without the contributions of the following data collection Partners from across the United States: | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
Alaska Department of Health Alaska Hospital and Healthcare Association Arizona Department of Health Services Arkansas Department of Health California Department of Health Care Access and Information Colorado Hospital Association Connecticut Hospital Association Delaware Division of Public Health District of Columbia Hospital Association Florida Agency for Health Care Administration Georgia Hospital Association Hawaii Laulima Data Alliance Hawaii University of Hawai'i at Hilo Illinois Department of Public Health Indiana Hospital Association Iowa Hospital Association Kansas Hospital Association Kentucky Cabinet for Health and Family Services Louisiana Department of Health Maine Health Data Organization Maryland Health Services Cost Review Commission Massachusetts Center for Health Information and Analysis Michigan Health & Hospital Association Minnesota Hospital Association Mississippi State Department of Health Missouri Hospital Industry Data Institute |
Montana Hospital Association Nebraska Hospital Association Nevada Department of Health and Human Services New Hampshire Department of Health & Human Services New Jersey Department of Health New Mexico Department of Health New York State Department of Health North Carolina Department of Health and Human Services North Dakota (data provided by the Minnesota Hospital Association) Ohio Hospital Association Oklahoma State Department of Health Oregon Association of Hospitals and Health Systems Oregon Health Authority Pennsylvania Health Care Cost Containment Council Rhode Island Department of Health South Carolina Revenue and Fiscal Affairs Office South Dakota Association of Healthcare Organizations Tennessee Hospital Association Texas Department of State Health Services Utah Department of Health Vermont Association of Hospitals and Health Systems Virginia Health Information Washington State Department of Health West Virginia Department of Health and Human Resources Wisconsin Department of Health Services Wyoming Hospital Association |
|
About the NIS
The HCUP National (Nationwide) Inpatient Sample (NIS) is a nationwide database of hospital inpatient stays. The NIS is nationally representative of all community hospitals (i.e., short-term, non-Federal, nonrehabilitation hospitals). The NIS includes all payers. It is drawn from a sampling frame that contains hospitals comprising more than 96 percent of all discharges in the United States. The vast size of the NIS allows the study of topics at the national and regional levels for specific subgroups of patients. In addition, NIS data are standardized across years to facilitate ease of use. Over time, the sampling frame for the NIS has changed; thus, the number of States contributing to the NIS varies from year to year. The NIS is intended for national estimates only; no State-level estimates can be produced. The unweighted sample size for the 2020 NIS is 6,471,165 (weighted, this represents 32,355,827 inpatient stays). For More Information For other information on hospitalizations related to mental health disorders and maternal health, refer to the Mental and Substance Use Disorders, Race and Ethnicity, Pregnancy and Childbirth, and Women's Health HCUP Statistical Briefs topic areas located at www.hcup-us.ahrq.gov/reports/statbriefs/sbtopic.jsp. For additional HCUP statistics, visit:
For a detailed description of HCUP and more information on the design of the National Inpatient Sample (NIS), please refer to the following database documentation: Agency for Healthcare Research and Quality. Overview of the National (Nationwide) Inpatient Sample (NIS). Healthcare Cost and Utilization Project (HCUP). Rockville, MD: Agency for Healthcare Research and Quality. Updated September 2021. www.hcup-us.ahrq.gov/nisoverview.jsp. Accessed March 9, 2022. Suggested Citation Weiss AJ (IBM), Head MA (IBM), Reid LD (AHRQ). Mental Health Disorders Among Delivery Inpatient Stays by Patient Race and Ethnicity, 2020. HCUP Statistical Brief #302. December 2022. Agency for Healthcare Research and Quality, Rockville, MD. www.hcup-us.ahrq.gov/reports/statbriefs/sb302-Deliveries-Mental-Health-Disorders-Race-2020.pdf. Acknowledgments The authors would like to acknowledge the contributions of Marguerite Barrett of M.L. Barrett, Inc., and Minya Sheng of IBM. *** AHRQ welcomes questions and comments from readers of this publication who are interested in obtaining more information about access, cost, use, financing, and quality of healthcare in the United States. We also invite you to tell us how you are using this Statistical Brief and other HCUP data and tools, and to share suggestions on how HCUP products might be enhanced to further meet your needs. Please email us at hcup@ahrq.gov or send a letter to the address below:Joel W. Cohen, Ph.D., Director Center for Financing, Access and Cost Trends Agency for Healthcare Research and Quality 5600 Fishers Lane Rockville, MD 20857 This Statistical Brief was posted online on December 13, 2022. a Agency for Healthcare Research and Quality. Clinical Classifications Software Refined (CCSR) for ICD-10-CM Diagnoses. Healthcare Cost and Utilization Project (HCUP). Agency for Healthcare Research and Quality. Updated February 2022. www.hcup-us.ahrq.gov/toolssoftware/ccsr/dxccsr.jsp. Accessed March 9, 2022. b Leonard SA, Kennedy CJ, Carmichael SL, Lyell DJ, Main EK. An expanded obstetric comorbidity scoring system for predicting severe maternal morbidity. Obstetrics & Gynecology. 2020;136(3):440–9. |
| Supplemental Table 1. Rate of delivery stays involving a mental health disorder diagnosis, by type of mental health disorder and patient race and ethnicity, 2020, for data presented in Figure 3 | ||||||
| Type of mental health disorder | Overall | API NH | Black NH | Hispanic | White NH | Other NH |
|---|---|---|---|---|---|---|
| Rate per 100 delivery stays | ||||||
| Anxiety and obsessive-compulsive disorders | 6.7 | 2.2 | 4.0 | 3.4 | 9.6 | 4.6 |
| Depressive disorders | 5.0 | 1.6 | 4.2 | 3.0 | 6.6 | 3.8 |
| Percent change vs. 2017 | ||||||
| Anxiety and obsessive-compulsive disorders | 74.3 | 100.4 | 78.9 | 75.8 | 73.6 | 93.3 |
| Depressive disorders | 61.3 | 74.5 | 55.2 | 60.3 | 63.2 | 93.4 |
| Internet Citation: Statistical Brief #302. Healthcare Cost and Utilization Project (HCUP). December 2022. Agency for Healthcare Research and Quality, Rockville, MD. hcup-us.ahrq.gov/reports/statbriefs/sb302-Deliveries-Mental-Health-Disorders-Race-2020.jsp. |
| Are you having problems viewing or printing pages on this website? |
| If you have comments, suggestions, and/or questions, please contact hcup@ahrq.gov. |
| If you are experiencing issues related to Section 508 accessibility of information on this website, please contact hcup@ahrq.gov. |
| Privacy Notice, Viewers & Players |
| Last modified 12/12/22 |